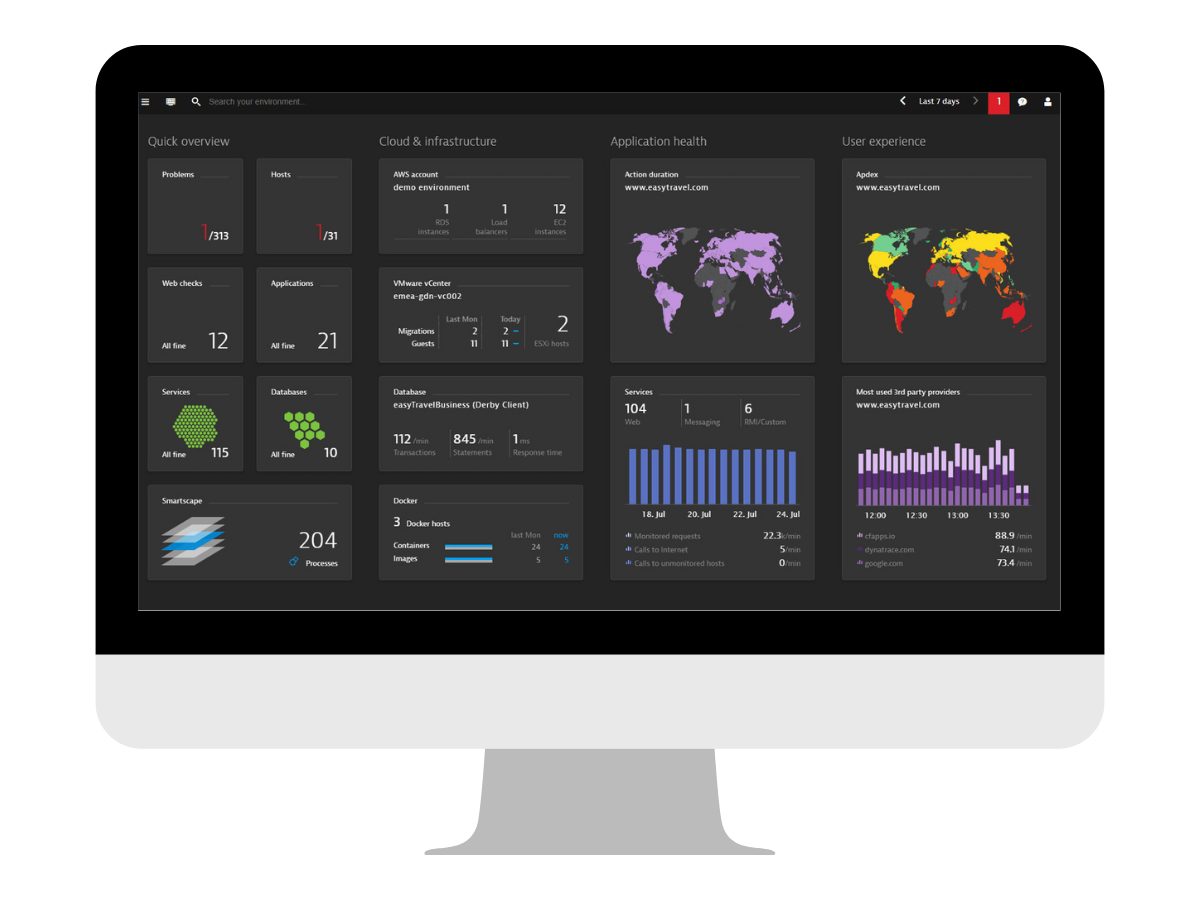
Dovera Insurance Company: Response Time for Troubleshooting Reduced with Application Monitoring
Dôvera Insurance Company needed to augment application monitoring with a tool that would be able to find the cause of the problem and its extent. In addition, the client required quality reporting of all events.
Background and Challenge
Know about application problems before a disgruntled client alerts you to them? That’s precisely what Dynatrace application monitoring helped Dôvera a.s. – health insurance company – do.
Thanks to it, the insurance company has significantly improved the customer experience of its insured.
Quickly find the cause of the problem
Full availability of applications at all times is one of the main tasks of the application and service support department of the IT department of the insurance company Dôvera.
If application performance falls below established metrics or fails, it is necessary to react quickly, identify the cause and reduce the response time to a minimum during the actual resolution.
Dôvera Insurance Company needed to augment application monitoring with a tool that would be able to find the cause of the problem and its extent.
In addition, the client required quality reporting of all events.
Dynatrace is a leader in application monitoring
Health insurance company Dôvera a.s. decided to implement the Dynatrace APM application tool. Gartner rates the tool as a leader in Application Performance Monitoring, which contributed to the decision.
Dynatrace provides a comprehensive overview of the client’s applications, identifies problems, and looks for their causes.
Solution
Dynatrace provides detail down to the user level
Impact
How has the insurance company improved the customer experience with Dynatrace’s application monitoring?
The Dynatrace APM tool was deployed to the client’s Employer Electronic Portal in Q1 2021. Once the monitored parameters have been debugged, IT support teams receive automatic alerts for any anomalies, malfunctions or slowdowns in processes, always with detailed identification of the cause.
As a result, the insurance company knows about application problems long before its clients start alerting it.
Based on the data collected, the insurance company was able to optimize the functionality of the applications. For example, it creates clear dashboards by individual metrics and can generate full reporting from the monitored data.